A HosCom International 2023 Vol. 1 Article
World Information
Challenges and Expriences of Handling COVID-19 in Penang Hospital, Malaysia
Authors:
Dr. Chuan Huan Chuah, Dr. Kar Nim Leong, Dr. Ting Soo Chow, Dr. Peng Shyan Wong
Hospital Pulau Penang
Introduction
Since the first reported COVID-19 case in Malaysia on 25th January 2020, all public hospitals, including Penang General Hospital, have been prepared for the outbreak. Confirmed COVID-19 cases were initially concentrated in Kuala Lumpur with the arrival of international travellers before spreading throughout the country, including Penang. Due to the increasing number of cases, the country was placed under a restrictive movement control order on 18th March 2020. The country faced the toughest challenge during the period between July and October 2021, when the number of cases rose above 20,000 per day, with many still not fully vaccinated against the virus.
Our Challenges
- Inadequate hospital beds in wards and ICUs
- Lack of manpower
- Low oxygen pressure within aging infrastructures
- Low PPE supply, particularly N95 masks
- Positive COVID-19 cases among healthcare staff
- Positive COVID-19 patients diagnosed in non-COVID-19 wards
- Vaccine hesitancy among the public and some healthcare staff
- New surge due to the Omicron variant
Our Experiences and Strategies
Preparation of healthcare facilities and manpower
During the early phase, the hospital director promptly called for meetings to bring in all relevant clinical and nonclinical departments, as well as infection control, nursing, and engineering representatives. This allowed for unified decision-making on how best to convert existing wards into COVID-19 wards, expand ICU services, and mobilise manpower. Staff members from other departments were deployed to join the COVID-19 team. Elective surgeries and nonurgent procedures were reduced and even stopped to handle the surge in COVID-19 cases.
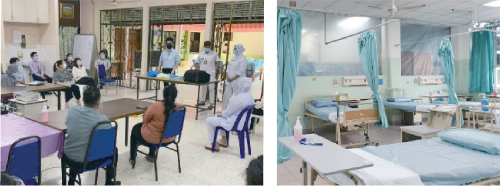
Setting up low-risk centres
In the initial phase, all positive COVID-19 patients were required to quarantine in healthcare facilities for monitoring. Several low-risk centres were set up at the hospital and state levels. There was also an outbreak of COVID-19 infections in the prison, which is located next to the hospital, in October 2020. Fortunately, most patients suffered only mild symptoms. Instead of bringing the patients into healthcare facilities, part of the prison was converted into a low-risk centre. Medical staff were deployed to monitor these patients on-site. The majority of the patients recovered without complications, and only a few needed to be transferred to hospital wards.

Handling the Delta wave
The most challenging period was from July to October 2021, when the Delta wave hit the country. Many patients were admitted with severe disease and required oxygen support and ICU care. More than 10 wards were repurposed to manage the surge in patients. Other intensive units (e.g., cardiology, cardiothoracic, and plastic surgery) were converted into COVID-19 ICUs to handle severe cases. With the help of the national armed forces, field hospitals were built in Kepala Batas Hospital and Penang General Hospital. These field hospitals were fully equipped with oxygen-capable beds and high-dependency units. Oxygen pressure was adequate to sustain multiple high-flow nasal cannula machines.

Waves and vaccines
During the peak, the federal government mobilised staff from the Klang Valley to Penang to assist. These individuals included specialists, medical doctors, and paramedics. The COVID-19 cases came in waves. When the numbers declined, the staff members were returned, and the repurposed wards were converted back to normal wards. This allowed the hospital to resume all essential services. Thanks to the rapid national immunization program, almost 80% of the population completed primary vaccination by November 2021. However, the uptake of booster doses was less than 50%. The country was subsequently hit with the Omicron wave, and the daily cases went back up. Fortunately, due to the high vaccination rates, the disease severity was mild, and most patients were allowed to quarantine at home.
Maintaining enough PPE
For PPE, there was no major disruption of supply to our hospital. The management team monitored the usage and supply during the peak. Apart from the supply from the ministry, we were fortunate to receive numerous donations of PPE from various channels. Donors included NGOs, private companies, and individuals. However, there were times when certain PPE items, like N95 masks, ran low. To manage this shortage, the staff members were reminded to avoid wastage.
Infection control in the hospital
Infection control is important not just in COVID-19 wards, but also in other non-COVID-19 areas. The infection control team performed regular training and supervision to reduce the risk of transmission in the ward. The hospital adopted a no-visitor policy during the pandemic. If caretakers or family members needed to be in the ward, the number was limited, and they were required to perform a self-test for COVID-19 whenever they entered the hospital. During the surge in cases, many healthcare workers were diagnosed with COVID-19. The majority of them had acquired the infection from the community. This led to manpower shortages and service disruptions. Measures taken to counter this problem included restricting the number of people eating together in the pantry, ensuring compliance with PPE, and using virtual platforms to conduct meetings and conferences.

NGO support
We were fortunate and grateful to receive significant support from NGOs. Donors connected directly with clinicians on the ground to understand their needs. Medical equipment and consumables were crucial due to the expansion of wards. Donated items included PPE, test kits, high-flow nasal cannula machines, oxygen concentrators, ultrasound machines, X-Ray machines, and laptops. We also received other forms of support, including food and moral support.
Recommendations
- Have a contingency plan for case surges
- Recruit more healthcare workers into the COVID-19 workforce
- Train more doctors, including specialists in managing severe and critical COVID-19 patients
- Increase surveillance testing in the hospital to diagnose positive cases earlier
- Improve oxygen pressure capacity in facilities
- Keep staff updated on the latest evidence in the management and infection control of COVID-19
- Maintain the welfare of frontliners
- Increase uptake for adult vaccine booster doses and primary doses for the paediatric population
-
Publication Date:March 04, 2023
-
Category:HAI
HosCom International 2023 Vol. 1
